Kidney Stones
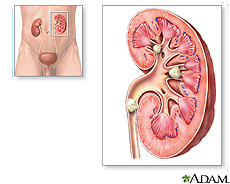
A kidney stone is a solid piece of material that forms in the kidney from substances in the urine. It may be as small as a grain of sand or as large as a pearl. Most kidney stones pass out of the body without help from a doctor. But sometimes a stone will not go away. It may get stuck in the urinary tract, block the flow of urine and cause great pain.
The following may be signs of kidney stones that need a doctor's help:
How does diet affect the risk of developing kidney stones? Diet is one of several factors that can promote or inhibit kidney stone formation. Other factors include heredity, environment, weight, and fluid intake. The body uses food for energy and tissue repair. After the body uses what it needs, waste products in the bloodstream are carried to the kidneys and excreted as urine. Certain foods create wastes that may form crystals in the urinary tract. In some people, the crystals grow into stones. For people who have had a kidney stone, preventing another will be a priority. In addition to dietary changes, a person may need medicine to prevent kidney stones. The first step in preventing kidney stones is to learn what kind of stones a person’s body typically makes.
What are the types of kidney stones?
How does a doctor determine the type of kidney stone? If a person can catch a kidney stone as it passes, the doctor can send the stone to a laboratory for analysis. For stones that are causing symptoms, the doctor may also retrieve a stone surgically or with a scope inserted through the urethra into the bladder or ureter.
The doctor will also order tests to look for unusual levels of chemicals such as calcium, oxalate, magnesium, and sodium in the blood and urine to help design a prevention strategy.
How much fluid should a person drink to prevent stone formation? The amount of fluid a person needs to drink depends on the weather and the person’s activity level. People who have had a kidney stone should drink enough water and other fluids to produce at least 2 quarts of urine a day. Some doctors have their patients collect urine for 24 hours so the volume can be measured. The doctor can then advise the patient about increasing fluid intake, if necessary. People who work or exercise in hot weather need more fluid to replace the fluid they lose through sweat. Drinking enough water helps keep urine diluted and flushes away materials that might form stones and is the most important thing a person can do to prevent kidney stones.
A person at risk for cystine stones should drink enough water each day to dilute the concentration of cystine that escapes into the urine, which may be difficult. More than a gallon of water may be needed every 24 hours.
What fluids protect against kidney stone formation? Water is an inexpensive and calorie-free protection against kidney stones.
Some studies suggest citrus drinks like lemonade and orange juice protect against stones because they contain citrate, which stops crystals from growing into stones. But no large-scale trials have been conducted to confirm these findings. While citrus drinks may be helpful in preventing calcium oxalate stones and uric acid stones, they might be harmful for people who form calcium phosphate stones.
Coffee and tea can add to a person’s total fluid intake and have been shown to reduce the risk of stone formation, but they do contain oxalate. Moderate intake of beer and wine may also protect against stone formation.
What fluids should be avoided? Grapefruit juice and dark colas have been found to increase the risk of stone formation and should be avoided by people who are prone to calcium oxalate stone formation. Although cranberry juice is often promoted as useful for preventing urinary tract infections, it contains oxalate and may be harmful to stone formers.
How does salt in the diet affect kidney stone formation? Salt is made up of sodium and chloride. The sodium in salt, when excreted by the kidneys, causes more calcium to be excreted into the urine. High concentrations of calcium in the urine combine with oxalate and phosphorus to form stones. Reducing salt intake is preferred to reducing calcium intake.
The U.S. recommended daily allowance (RDA) of sodium is 2,400 milligrams (mg), but Americans’ intake averages 3,300 mg, according to the National Heart, Lung, and Blood Institute. The risk of kidney stones increases with increased daily sodium consumption. Limiting salt to the U.S. RDA goal of 2,400 mg is an important step for people who form calcium oxalate or calcium phosphate stones. People taking medications—such as hydrochlorothiazide, chlorthalidone, or indapamide—to prevent stones still need to limit salt intake.
How can a person limit sodium intake? Learning the sodium content of foods can help people control their sodium intake. Food labels provide information about sodium and other nutrients. Keeping a sodium diary can help a person limit sodium intake to 2,400 mg. When eating out, people should ask about the sodium content of foods they order.
Some foods have such large amounts of sodium that a single serving provides a major portion of the daily allowance. Foods that contain high levels of sodium include
Nondairy animal proteins may also increase the risk of calcium stones by increasing the excretion of calcium and reducing the excretion of citrate into the urine. Citrate prevents kidney stones, but the acid in animal protein reduces the citrate in urine.
How does calcium in the diet affect kidney stone formation? Calcium from food does not increase the risk of calcium oxalate stones. Calcium in the digestive tract binds to oxalate from food and keeps it from entering the blood, and then the urinary tract, where it can form stones. People who form calcium oxalate stones should include 800 mg of calcium in their diet every day, not only for kidney stone prevention but also to maintain bone density. A cup of low-fat milk contains 300 mg of calcium. Other dairy products such as yogurt are also high in calcium. For people who have lactose intolerance and must avoid dairy products, orange juice fortified with calcium or dairy with reduced lactose content may be alternatives. Some studies indicate that calcium supplements increase the risk of calcium oxalate stone formation. Researchers theorize that calcium must be taken at the same time as dietary oxalate to protect against stone formation. Calcium supplements taken with meals may have the same protective effect as dietary calcium
How does oxalate in the diet affect kidney stone formation? Some of the oxalate in urine is made by the body. But eating certain foods with high levels of oxalate can increase the amount of oxalate in the urine, where it combines with calcium to form calcium oxalate stones.
How can a person limit oxalate in the urine? Many foods and beverages contain oxalate, but only a few have been shown to increase the amount of oxalate in urine:
How does alcohol affect kidney stone formation? Although drinking alcohol may promote purine production in the body, studies have not shown more stones in people who drink beer and wine. People should have no more than two drinks—two 12-ounce servings of beer or two 5-ounce servings of wine or two 1.5-ounce servings of hard liquor—a day.
How do supplements affect kidney stone formation? Supplements containing vitamin C or D may contribute to stone formation. Vitamin C is ascorbate and can be turned into oxalate by the body. Doctors recommend no more than 500 milligrams each day for people who have had kidney stones. Calcium supplements should be taken with meals so the calcium can bind with the oxalate in food. A person who has a tendency to form kidney stones should consult a doctor or dietitian before taking large doses of vitamins or minerals.
How does a person’s weight affect kidney stone formation? Studies have shown that being overweight increases the risk of uric acid and calcium kidney stones. Scientists don’t know whether losing weight by itself can reduce the risk of kidney stones. Maintaining a healthy weight through healthy food choices and exercise may help reduce the risk of kidney stones.
Can a dietitian help a person prevent kidney stones? Yes. After a doctor has completed an evaluation and determined the causes of a person’s stones, a dietitian can help a person plan meals that lower the risk of forming stones. People who form stones can ask their doctor or nurse to help them find a dietitian who specializes in kidney stone prevention or renal, or kidney, nutrition.
The following may be signs of kidney stones that need a doctor's help:
- Extreme pain in your back or side that will not go away
- Blood in your urine
- Fever and chills
- Vomiting
- Urine that smells bad or looks cloudy
- A burning feeling when you urinate
How does diet affect the risk of developing kidney stones? Diet is one of several factors that can promote or inhibit kidney stone formation. Other factors include heredity, environment, weight, and fluid intake. The body uses food for energy and tissue repair. After the body uses what it needs, waste products in the bloodstream are carried to the kidneys and excreted as urine. Certain foods create wastes that may form crystals in the urinary tract. In some people, the crystals grow into stones. For people who have had a kidney stone, preventing another will be a priority. In addition to dietary changes, a person may need medicine to prevent kidney stones. The first step in preventing kidney stones is to learn what kind of stones a person’s body typically makes.
What are the types of kidney stones?
- Calcium oxalate stones are the most common. They tend to form when the urine is acidic, meaning it has a low pH. Some of the oxalate in urine is produced by the body. Calcium and oxalate in the diet play a part but are not the only factors that affect the formation of calcium oxalate stones. Dietary oxalate is an organic molecule found in many vegetables, fruits, and nuts. Calcium from bone may also play a role in kidney stone formation.
- Calcium phosphate stones are less common. Calcium phosphate stones tend to form when the urine is alkaline, meaning it has a high pH.
- Uric acid stones are more likely to form when the urine is persistently acidic, which may result from a diet rich in animal proteins and purines—substances found naturally in all food but especially in organ meats, fish, and shellfish.
- Struvite stones result from infections in the kidney. Preventing struvite stones depends on staying infection free. Diet has not been shown to affect struvite stone formation.
- Cystine stones result from a rare genetic disorder that causes cystine—an amino acid, one of the building blocks of protein—to leak through the kidneys and into the urine to form crystals.
- Why is knowing which type of stone a person has important? Knowing the chemical makeup of the stone helps the doctor identify why the patient is prone to stone formation. The kind of stone a person’s body makes determines what dietary changes may be needed. For example, limiting oxalate in the diet may help prevent calcium oxalate stones but will do nothing to prevent uric acid stones. Some dietary recommendations may apply to more than one type of stone. Most notably, drinking enough water helps prevent all kinds of kidney stones.
How does a doctor determine the type of kidney stone? If a person can catch a kidney stone as it passes, the doctor can send the stone to a laboratory for analysis. For stones that are causing symptoms, the doctor may also retrieve a stone surgically or with a scope inserted through the urethra into the bladder or ureter.
The doctor will also order tests to look for unusual levels of chemicals such as calcium, oxalate, magnesium, and sodium in the blood and urine to help design a prevention strategy.
How much fluid should a person drink to prevent stone formation? The amount of fluid a person needs to drink depends on the weather and the person’s activity level. People who have had a kidney stone should drink enough water and other fluids to produce at least 2 quarts of urine a day. Some doctors have their patients collect urine for 24 hours so the volume can be measured. The doctor can then advise the patient about increasing fluid intake, if necessary. People who work or exercise in hot weather need more fluid to replace the fluid they lose through sweat. Drinking enough water helps keep urine diluted and flushes away materials that might form stones and is the most important thing a person can do to prevent kidney stones.
A person at risk for cystine stones should drink enough water each day to dilute the concentration of cystine that escapes into the urine, which may be difficult. More than a gallon of water may be needed every 24 hours.
What fluids protect against kidney stone formation? Water is an inexpensive and calorie-free protection against kidney stones.
Some studies suggest citrus drinks like lemonade and orange juice protect against stones because they contain citrate, which stops crystals from growing into stones. But no large-scale trials have been conducted to confirm these findings. While citrus drinks may be helpful in preventing calcium oxalate stones and uric acid stones, they might be harmful for people who form calcium phosphate stones.
Coffee and tea can add to a person’s total fluid intake and have been shown to reduce the risk of stone formation, but they do contain oxalate. Moderate intake of beer and wine may also protect against stone formation.
What fluids should be avoided? Grapefruit juice and dark colas have been found to increase the risk of stone formation and should be avoided by people who are prone to calcium oxalate stone formation. Although cranberry juice is often promoted as useful for preventing urinary tract infections, it contains oxalate and may be harmful to stone formers.
How does salt in the diet affect kidney stone formation? Salt is made up of sodium and chloride. The sodium in salt, when excreted by the kidneys, causes more calcium to be excreted into the urine. High concentrations of calcium in the urine combine with oxalate and phosphorus to form stones. Reducing salt intake is preferred to reducing calcium intake.
The U.S. recommended daily allowance (RDA) of sodium is 2,400 milligrams (mg), but Americans’ intake averages 3,300 mg, according to the National Heart, Lung, and Blood Institute. The risk of kidney stones increases with increased daily sodium consumption. Limiting salt to the U.S. RDA goal of 2,400 mg is an important step for people who form calcium oxalate or calcium phosphate stones. People taking medications—such as hydrochlorothiazide, chlorthalidone, or indapamide—to prevent stones still need to limit salt intake.
How can a person limit sodium intake? Learning the sodium content of foods can help people control their sodium intake. Food labels provide information about sodium and other nutrients. Keeping a sodium diary can help a person limit sodium intake to 2,400 mg. When eating out, people should ask about the sodium content of foods they order.
Some foods have such large amounts of sodium that a single serving provides a major portion of the daily allowance. Foods that contain high levels of sodium include
- hot dogs
- canned soups and vegetables
- processed frozen foods
- luncheon meats
- fast food
- monosodium glutamate (MSG)
- sodium bicarbonate, the chemical name for baking soda
- baking powder, which contains sodium bicarbonate and other chemicals
- disodium phosphate
- sodium alginate
- sodium nitrate or nitrite
Nondairy animal proteins may also increase the risk of calcium stones by increasing the excretion of calcium and reducing the excretion of citrate into the urine. Citrate prevents kidney stones, but the acid in animal protein reduces the citrate in urine.
How does calcium in the diet affect kidney stone formation? Calcium from food does not increase the risk of calcium oxalate stones. Calcium in the digestive tract binds to oxalate from food and keeps it from entering the blood, and then the urinary tract, where it can form stones. People who form calcium oxalate stones should include 800 mg of calcium in their diet every day, not only for kidney stone prevention but also to maintain bone density. A cup of low-fat milk contains 300 mg of calcium. Other dairy products such as yogurt are also high in calcium. For people who have lactose intolerance and must avoid dairy products, orange juice fortified with calcium or dairy with reduced lactose content may be alternatives. Some studies indicate that calcium supplements increase the risk of calcium oxalate stone formation. Researchers theorize that calcium must be taken at the same time as dietary oxalate to protect against stone formation. Calcium supplements taken with meals may have the same protective effect as dietary calcium
How does oxalate in the diet affect kidney stone formation? Some of the oxalate in urine is made by the body. But eating certain foods with high levels of oxalate can increase the amount of oxalate in the urine, where it combines with calcium to form calcium oxalate stones.
How can a person limit oxalate in the urine? Many foods and beverages contain oxalate, but only a few have been shown to increase the amount of oxalate in urine:
- spinach
- rhubarb
- nuts
- wheat bran
How does alcohol affect kidney stone formation? Although drinking alcohol may promote purine production in the body, studies have not shown more stones in people who drink beer and wine. People should have no more than two drinks—two 12-ounce servings of beer or two 5-ounce servings of wine or two 1.5-ounce servings of hard liquor—a day.
How do supplements affect kidney stone formation? Supplements containing vitamin C or D may contribute to stone formation. Vitamin C is ascorbate and can be turned into oxalate by the body. Doctors recommend no more than 500 milligrams each day for people who have had kidney stones. Calcium supplements should be taken with meals so the calcium can bind with the oxalate in food. A person who has a tendency to form kidney stones should consult a doctor or dietitian before taking large doses of vitamins or minerals.
How does a person’s weight affect kidney stone formation? Studies have shown that being overweight increases the risk of uric acid and calcium kidney stones. Scientists don’t know whether losing weight by itself can reduce the risk of kidney stones. Maintaining a healthy weight through healthy food choices and exercise may help reduce the risk of kidney stones.
Can a dietitian help a person prevent kidney stones? Yes. After a doctor has completed an evaluation and determined the causes of a person’s stones, a dietitian can help a person plan meals that lower the risk of forming stones. People who form stones can ask their doctor or nurse to help them find a dietitian who specializes in kidney stone prevention or renal, or kidney, nutrition.
Kidney Diseases
Your kidneys are two bean-shaped organs, each about the size of your fists. They are located near the middle of your back, just below the rib cage. Inside each kidney about a million tiny structures called nephrons filter blood. They remove waste products and extra water, which become urine. The urine flows through tubes called ureters to your bladder, which stores the urine until you go to the bathroom.
Damage to the nephrons results in kidney disease. This damage may leave kidneys unable to remove wastes. Usually the damage occurs slowly over years. There are no obvious symptoms, so you don't know it is happening.
Many things can cause kidney disease. You are at risk if you have
Damage to the nephrons results in kidney disease. This damage may leave kidneys unable to remove wastes. Usually the damage occurs slowly over years. There are no obvious symptoms, so you don't know it is happening.
Many things can cause kidney disease. You are at risk if you have
- Diabetes
- High blood pressure
- A close family member with kidney disease
Kidney Failure
Healthy kidneys clean your blood by removing excess fluid, minerals and wastes. They also make hormones that keep your bones strong and your blood healthy. But if the kidneys are damaged, they don't work properly. Harmful wastes can build up in your body. Your blood pressure may rise. Your body may retain excess fluid and not make enough red blood cells. This is called kidney failure.
If your kidneys fail, you need treatment to replace the work they normally do. The treatment options are dialysis or a kidney transplant. Each treatment has benefits and drawbacks. No matter which treatment you choose, you'll need to make some changes in your life, including how you eat and plan your activities. But with the help of healthcare providers, family and friends, most people with kidney failure can lead full and active lives.
If your kidneys fail, you need treatment to replace the work they normally do. The treatment options are dialysis or a kidney transplant. Each treatment has benefits and drawbacks. No matter which treatment you choose, you'll need to make some changes in your life, including how you eat and plan your activities. But with the help of healthcare providers, family and friends, most people with kidney failure can lead full and active lives.
Kidney Transplantation
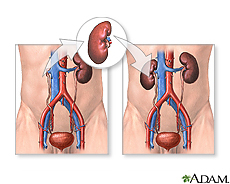
A kidney transplant is an operation that places a healthy kidney in your body. The transplanted kidney takes over the work of the two kidneys that failed, and you no longer need dialysis.
During a transplant, the surgeon places the new kidney in your lower abdomen and connects the artery and vein of the new kidney to your artery and vein. Often, the new kidney will start making urine as soon as your blood starts flowing through it. But sometimes it takes a few weeks to start working.
Many transplanted kidneys come from donors who have died. Some come from a living family member. The wait for a new kidney can be long. People who have transplants must take drugs to keep their body from rejecting the new kidney for the rest of their lives.
During a transplant, the surgeon places the new kidney in your lower abdomen and connects the artery and vein of the new kidney to your artery and vein. Often, the new kidney will start making urine as soon as your blood starts flowing through it. But sometimes it takes a few weeks to start working.
Many transplanted kidneys come from donors who have died. Some come from a living family member. The wait for a new kidney can be long. People who have transplants must take drugs to keep their body from rejecting the new kidney for the rest of their lives.
Kidney Cancer
You have two kidneys. They are fist-sized organs on either side of your backbone above your waist. The tubes inside filter and clean your blood, taking out waste products and making urine. Kidney cancer forms in the lining of tiny tubes inside your kidneys. It happens most often in people over 40. Risk factors include smoking, having certain genetic conditions and misusing pain medicines for a long time.
Often, kidney cancer doesn't have early symptoms. However, see your health care provider if you notice
Often, kidney cancer doesn't have early symptoms. However, see your health care provider if you notice
- Blood in your urine
- A lump in your abdomen
- Unexplained weight loss
- Pain in your side
- Loss of appetite
Renal Artery Stenosis
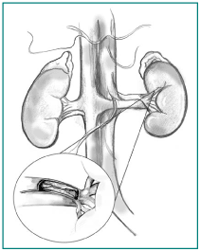
Renal artery stenosis (RAS) is the narrowing of one or both arteries that carry blood to the two kidneys. "Renal" means "kidney" and "stenosis" means "narrowing." RAS can cause high blood pressure and reduce kidney function. RAS is often overlooked as a cause of high blood pressure.
You are at greater risk of developing RAS if you smoke or are overweight. RAS is most common in men between the ages of 50 and 70, but women and younger adults can also have it. High cholesterol, diabetes, and a family history of cardiovascular disease are also risk factors for RAS. High blood pressure is both a cause and result of RAS.
What are the kidneys? Your two kidneys are bean-shaped organs, each about the size of a fist. They are located just below the rib cage, one on each side of the spine. The arteries that carry blood to the kidneys-called the renal arteries-branch off directly from the abdominal aorta, the main vessel from the heart that supplies blood to most of the body's organs.
Healthy kidneys filter out wastes and extra fluid from the blood that passes through them. Those wastes and extra fluid become urine, which flows from the kidneys to the bladder through tubes called ureters. Urine is stored in the bladder until released through urination.
What causes RAS? In an overwhelming majority of cases, RAS is caused by atherosclerosis, hardening of the kidney arteries. Thus, RAS develops when a material called plaque builds up on the inner wall of one or both of the renal arteries. The plaque makes the artery wall hard and narrow. This narrowing reduces or cuts off the blood supply, possibly damaging the kidney. The damaged kidney is less efficient at removing wastes and extra fluid from the blood. This plaque is similar to plaques blocking the arteries supplying the heart, which cause heart attacks, and those blocking arteries supplying the brain, which cause strokes.
When the kidneys fail, wastes and extra fluid build up in the blood. This condition, called uremia, causes nausea, headaches, fatigue, and swelling in the legs and abdomen. With total kidney failure, you will need dialysis or a kidney transplant to stay alive.
What are the symptoms of RAS? RAS can be silent, meaning you will not feel any symptoms, until it becomes severe.
The first sign of RAS may be high blood pressure that stays high even when you take blood pressure medicine. High blood pressure caused by RAS is called renovascular hypertension. Your doctor cannot diagnose RAS based on blood pressure alone because many conditions can cause your blood pressure to rise. If you develop high blood pressure suddenly and have no family history of high blood pressure, or if your blood pressure is difficult to control, your doctor might suspect RAS.
How is RAS diagnosed? When blood flows through a narrow vessel, it makes a whooshing sound, called a bruit (BROO-ee). Your doctor may place a stethoscope on the front or the side of your abdomen to listen for this sound. The absence of this sound, however, by no means excludes the possibility of RAS.
For a more accurate diagnosis, your doctor may order an ultrasound or an angiogram to get a picture of the artery. An ultrasound uses harmless sound waves to create images of internal organs; it does not require intravenous injection or oral administration of any substances. An angiogram is a special kind of x ray in which a thin, flexible tube called a catheter is threaded through the large arteries, often from the groin, to the artery of interest-in this case, the renal artery. A special dye is injected through the catheter so the renal artery will show up clearer on the x ray. The advantage of angiograms is that they give a better picture and therefore more accurate diagnosis of RAS; the disadvantage is that this procedure is more invasive.
More recently, doctors have been using computerized tomography (CT) scans and magnetic resonance angiograms (MRA) to evaluate RAS. CT scans use multiple x-ray images combined by a computer to create a three-dimensional image of your internal organs. MRAs use moving magnets to create similar three-dimensional images. CT scans and MRAs are less invasive than conventional angiograms, but the results may not be as clear or accurate. Researchers are exploring ways to improve these imaging techniques and make them more reliable for evaluating RAS.
How is RAS treated? Approaches to RAS are threefold:
Blood Pressure Medicines RAS causes high blood pressure, which can damage the kidneys. Damaged kidneys, in turn, can make your blood pressure even higher. If left uncontrolled, this vicious cycle can lead to kidney failure and damage the heart and blood vessels throughout the body.
Controlling renovascular hypertension is often difficult but usually achievable. It may require two or more different kinds of blood pressure medicine. Blood pressure medicines work in different ways.
Sometimes, by combining two or more blood pressure medicines that work in different ways, you may be able to control your blood pressure and stop the progression of kidney failure. Each type of blood pressure medicine has its own potential side effects; therefore, the choice of medicine is best determined by you and your doctor.
In addition to blood pressure medicines, your doctor may prescribe a cholesterol lowering drug to prevent the plaques from forming in the arteries, and a blood-thinner, such as aspirin, to help the blood flow more easily through the arteries.
Surgery If RAS advances until the artery is nearly or completely blocked, you may need surgery to open up the flow of blood to the kidney. Different types of surgery for RAS include the following:
You are at greater risk of developing RAS if you smoke or are overweight. RAS is most common in men between the ages of 50 and 70, but women and younger adults can also have it. High cholesterol, diabetes, and a family history of cardiovascular disease are also risk factors for RAS. High blood pressure is both a cause and result of RAS.
What are the kidneys? Your two kidneys are bean-shaped organs, each about the size of a fist. They are located just below the rib cage, one on each side of the spine. The arteries that carry blood to the kidneys-called the renal arteries-branch off directly from the abdominal aorta, the main vessel from the heart that supplies blood to most of the body's organs.
Healthy kidneys filter out wastes and extra fluid from the blood that passes through them. Those wastes and extra fluid become urine, which flows from the kidneys to the bladder through tubes called ureters. Urine is stored in the bladder until released through urination.
What causes RAS? In an overwhelming majority of cases, RAS is caused by atherosclerosis, hardening of the kidney arteries. Thus, RAS develops when a material called plaque builds up on the inner wall of one or both of the renal arteries. The plaque makes the artery wall hard and narrow. This narrowing reduces or cuts off the blood supply, possibly damaging the kidney. The damaged kidney is less efficient at removing wastes and extra fluid from the blood. This plaque is similar to plaques blocking the arteries supplying the heart, which cause heart attacks, and those blocking arteries supplying the brain, which cause strokes.
When the kidneys fail, wastes and extra fluid build up in the blood. This condition, called uremia, causes nausea, headaches, fatigue, and swelling in the legs and abdomen. With total kidney failure, you will need dialysis or a kidney transplant to stay alive.
What are the symptoms of RAS? RAS can be silent, meaning you will not feel any symptoms, until it becomes severe.
The first sign of RAS may be high blood pressure that stays high even when you take blood pressure medicine. High blood pressure caused by RAS is called renovascular hypertension. Your doctor cannot diagnose RAS based on blood pressure alone because many conditions can cause your blood pressure to rise. If you develop high blood pressure suddenly and have no family history of high blood pressure, or if your blood pressure is difficult to control, your doctor might suspect RAS.
How is RAS diagnosed? When blood flows through a narrow vessel, it makes a whooshing sound, called a bruit (BROO-ee). Your doctor may place a stethoscope on the front or the side of your abdomen to listen for this sound. The absence of this sound, however, by no means excludes the possibility of RAS.
For a more accurate diagnosis, your doctor may order an ultrasound or an angiogram to get a picture of the artery. An ultrasound uses harmless sound waves to create images of internal organs; it does not require intravenous injection or oral administration of any substances. An angiogram is a special kind of x ray in which a thin, flexible tube called a catheter is threaded through the large arteries, often from the groin, to the artery of interest-in this case, the renal artery. A special dye is injected through the catheter so the renal artery will show up clearer on the x ray. The advantage of angiograms is that they give a better picture and therefore more accurate diagnosis of RAS; the disadvantage is that this procedure is more invasive.
More recently, doctors have been using computerized tomography (CT) scans and magnetic resonance angiograms (MRA) to evaluate RAS. CT scans use multiple x-ray images combined by a computer to create a three-dimensional image of your internal organs. MRAs use moving magnets to create similar three-dimensional images. CT scans and MRAs are less invasive than conventional angiograms, but the results may not be as clear or accurate. Researchers are exploring ways to improve these imaging techniques and make them more reliable for evaluating RAS.
How is RAS treated? Approaches to RAS are threefold:
- preventing RAS from getting worse
- treating high blood pressure that results from RAS
- relieving the blockage of the renal arteries
Blood Pressure Medicines RAS causes high blood pressure, which can damage the kidneys. Damaged kidneys, in turn, can make your blood pressure even higher. If left uncontrolled, this vicious cycle can lead to kidney failure and damage the heart and blood vessels throughout the body.
Controlling renovascular hypertension is often difficult but usually achievable. It may require two or more different kinds of blood pressure medicine. Blood pressure medicines work in different ways.
Sometimes, by combining two or more blood pressure medicines that work in different ways, you may be able to control your blood pressure and stop the progression of kidney failure. Each type of blood pressure medicine has its own potential side effects; therefore, the choice of medicine is best determined by you and your doctor.
In addition to blood pressure medicines, your doctor may prescribe a cholesterol lowering drug to prevent the plaques from forming in the arteries, and a blood-thinner, such as aspirin, to help the blood flow more easily through the arteries.
Surgery If RAS advances until the artery is nearly or completely blocked, you may need surgery to open up the flow of blood to the kidney. Different types of surgery for RAS include the following:
- Angioplasty and stenting. Angioplasty is a procedure in which a catheter is put into the renal artery, usually through the groin, just as in a conventional angiogram. In addition, for angioplasty, a tiny balloon at the end of the catheter can be inflated to flatten the plaque against the wall of the artery. Then your doctor may position a small mesh tube, called a stent, to keep plaque flattened and the artery open.
- Endarterectomy. In an endarterectomy, a vascular surgeon cleans out the plaque, leaving the inside lining of the artery smooth and clear.
- Bypass surgery. To create a bypass, a vascular surgeon uses a vein or synthetic tube to connect the kidney to the aorta. This new path serves as an alternate route for blood to flow around the blocked artery into the kidney.
